-
-
How can I differentiate between a regular headache and a whiplash headache?
-
When should I seek medical help for chronic headaches following an injury?
-
What diagnostic tests are commonly used to identify whiplash-related headaches?
-
Are there non-pharmacological treatment options available for managing whiplash headaches?
Chronic headaches can be a debilitating condition, impacting daily life and productivity. Often stemming from factors like stress, poor posture, or underlying health issues, headache pain can cause whiplash patients, they require careful management for relief. On the other hand, whiplash, commonly associated with car accidents, can cause persistent neck pain and discomfort if not addressed promptly by patients experiencing head injury. Understanding the causes and treatments for these conditions is crucial in finding effective solutions and improving overall well-being.
Key Takeaways
-
Early Recognition: Promptly identifying whiplash headaches can lead to timely treatment and better outcomes.
-
Understanding the Root Causes: Delve into the underlying reasons for whiplash headaches to address them effectively.
-
Seeking Proper Diagnosis: A thorough diagnostic process is crucial in determining the best course of action for managing chronic headaches.
-
Tailored Treatments: Personalized treatment plans based on diagnosis can significantly alleviate whiplash headache symptoms.
-
Multidisciplinary Approach: Combining therapies like physical therapy, medications, and lifestyle modifications can enhance the effectiveness of treatment.
-
Regular Follow-ups: Scheduled check-ins with healthcare providers can track progress and make necessary adjustments to the treatment plan.
Recognizing Whiplash Headache

Key Symptoms
Whiplash headaches typically manifest as pain in the neck and head regions, often radiating to the shoulders. Patients may also experience stiffness in the neck muscles. The intensity of pain can vary from mild discomfort to severe throbbing sensations.
Patients with whiplash injuries may exhibit different patterns of pain intensity. Some individuals, patients, report constant dull aches, while others describe sharp, shooting pains. Understanding these variations is crucial for accurate diagnosis and treatment.
Dizziness is a common symptom associated with cervicogenic headaches, which are often linked to whiplash injuries. Patients experiencing dizziness alongside headache pain should seek medical evaluation to determine the underlying cause.
Onset Timing
Evaluating whiplash headaches promptly after an injury is crucial. Symptoms may appear immediately following the incident or develop gradually over hours or days. Early symptoms such as neck stiffness and headache are indicative of potential chronic issues.
Differentiating between early symptoms and chronic manifestations is essential for effective treatment planning. Early intervention can prevent the progression of symptoms into long-term chronic headache conditions, highlighting the importance of timely evaluation.
Prompt evaluation of whiplash headaches enables healthcare providers to assess the extent of injury accurately. This assessment guides the development of tailored treatment strategies that address both immediate pain relief and long-term management approaches for patients.
Severity and Duration
Assessing the severity of whiplash headaches involves evaluating pain intensity levels reported by patients. Severe headaches that significantly impact daily activities indicate a more acute condition requiring immediate attention.
Symptoms post-whiplash injury can vary in duration from weeks to months or even years for some patients. Understanding the prolonged nature of these symptoms is essential for implementing comprehensive treatment plans that address both short-term relief and long-term management strategies.
Treatment approaches for acute whiplash headaches differ from those used for chronic cases. Acute conditions often require immediate pain management techniques, while chronic cases necessitate long-term solutions focusing on symptom control and prevention strategies.
Unveiling the Causes
Neck Damage
Neck injuries are common culprits behind chronic headaches, with whiplash being a primary trigger among patients. Upper joint injuries, such as in the cervical spine, can lead to persistent headaches. Disc injuries in the upper neck region also play a significant role in causing chronic headaches.
Neurovascular Issues
Whiplash headaches can result in neurovascular complications, impacting blood vessels and nerves. Facet joint injuries from whiplash can affect neurovascular structures, exacerbating headache symptoms. Disc injuries in the upper neck area may manifest as neurovascular symptoms due to nerve compression.
Autonomic Dysfunction
Patients with whiplash headaches may exhibit signs of autonomic dysfunction, affecting bodily functions like heart rate and blood pressure regulation. Autonomic dysfunction can intensify headache severity by influencing pain perception and vascular changes. Addressing autonomic dysfunction is crucial in comprehensive treatment plans for chronic headaches in patients.
Proprioception Problems
Individuals with whiplash headaches often face challenges related to proprioception, the body’s sense of self-movement and position. Proprioception issues can worsen headache symptoms by disrupting coordination and balance. Neck exercises play a pivotal role in enhancing proprioception, ultimately reducing headache frequency and intensity in patients.
Diagnostic Journey
Initial Evaluation
During the initial evaluation, healthcare providers emphasize a thorough physical examination to diagnose whiplash headaches accurately. This involves assessing neck mobility, tenderness, and muscle spasms. Evaluating neurological symptoms like tingling or numbness is crucial.
Typical pain patterns observed during the initial evaluation include neck stiffness, radiating pain to the shoulders, and headaches that worsen with movement. Patients often report these symptoms following a car accident or sudden impact.
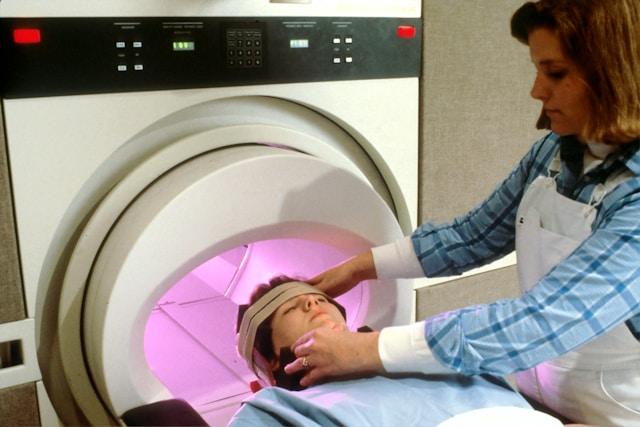
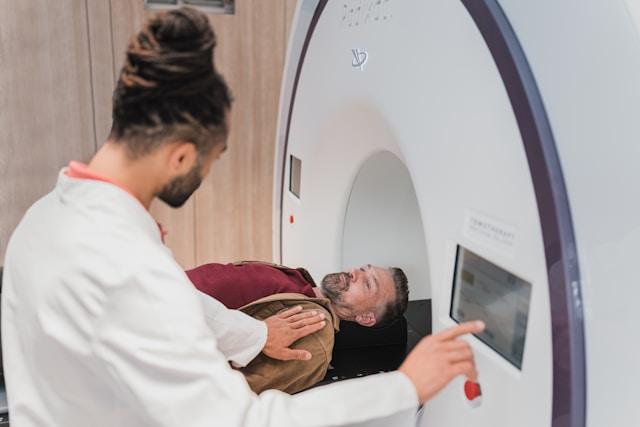
An MRI plays a vital role in identifying disc herniation post-whiplash injury. It provides detailed images of the cervical spine, helping healthcare professionals pinpoint any structural abnormalities that could be contributing to the headaches.
Advanced Testing
Beyond MRI, additional diagnostic testing may be necessary to diagnose facet joint injuries accurately. These tests can include CT scans or specialized imaging studies to visualize the facet joints in more detail.
Diagnostic injections such as medial branch blocks are essential for confirming facet joint involvement in whiplash-related headaches. By injecting medication around the medial branches of spinal nerves, doctors can determine if these nerves are contributing to the pain.
Advanced testing techniques are instrumental in confirming specific neck injuries that may be causing chronic headaches post-whiplash. These tests provide detailed insights into soft tissue damage, nerve compression, or joint abnormalities.
Severity Assessment
Healthcare providers assess the severity of whiplash headaches based on diagnostic findings from physical exams and imaging studies. Understanding the extent of tissue damage and nerve involvement helps determine the appropriate treatment approach.
Facet joint injuries can significantly impact headache severity by causing referred pain patterns and exacerbating existing symptoms. Identifying these injuries early on is crucial for managing pain effectively and preventing long-term complications.
Personalized treatment plans are essential for addressing whiplash headache severity effectively. By tailoring therapies to each patient’s specific needs and symptoms, healthcare providers can optimize outcomes and improve quality of life.
Treatment Pathways
Medical Interventions
Nonsteroidal anti-inflammatory medications can effectively reduce pain and inflammation associated with whiplash headaches. Muscle relaxants play a crucial role in managing headache symptoms by helping to alleviate muscle tension and spasms. In severe cases, spinal injections may be necessary to provide targeted pain relief and reduce inflammation in the facet joints.
Physical Therapy
Therapy and neck exercises are essential in the initial treatment of whiplash headaches as they aid in restoring neck mobility and strengthening supporting muscles. Physical therapy can significantly improve neck flexibility, decrease pain levels, and enhance overall function. Exercise programs designed to strengthen neck muscles can also play a vital role in preventing the development of chronic headaches.
Home Remedies
Using heat or ice packs can provide relief from whiplash headache symptoms by reducing inflammation and soothing sore muscles. Maintaining good posture is crucial in minimizing neck strain, which can exacerbate headache intensity. Incorporating relaxation techniques such as deep breathing exercises or meditation can help manage headache intensity by reducing stress levels.
Lifestyle Adjustments
Lifestyle modifications such as ensuring proper ergonomics at workstations and during activities can help prevent whiplash headaches by reducing strain on the neck muscles. Effective stress management techniques like regular exercise or mindfulness practices can significantly impact the frequency and severity of headaches. Making ergonomic adjustments like using supportive pillows or chairs can also aid in reducing neck strain and decreasing the occurrence of headaches.
Closing Thoughts
Understanding the signs of whiplash headaches, delving into their root causes, navigating the diagnostic process, and exploring treatment options have equipped you with valuable insights. By recognizing the symptoms early on, you can seek timely medical attention and appropriate care tailored to your needs. Remember, knowledge is power when it comes to managing chronic headaches resulting from whiplash injuries.
As you continue your journey towards relief and recovery, stay proactive in communicating with healthcare professionals, following treatment plans diligently, and exploring complementary therapies. Your commitment to self-care and well-being will play a pivotal role in alleviating symptoms and enhancing your quality of life. Take charge of your health and seek support whenever needed to overcome the challenges posed by whiplash-related headaches.
Frequently Asked Questions
What are the common symptoms of whiplash headaches?
Whiplash headaches often present with symptoms like neck pain, stiffness, dizziness, blurred vision, and persistent headaches that radiate from the base of the skull towards the forehead.
How can I differentiate between a regular headache and a whiplash headache, considering associated symptoms?
A key differentiator is that whiplash headaches typically occur after a traumatic event like a car accident or sports injury. They are often accompanied by neck pain and stiffness, unlike regular headaches.
When should whiplash patients seek medical help for chronic headaches and associated symptoms following an injury?
If you experience persistent or worsening headaches after an injury, especially if they are accompanied by other symptoms like neck pain or dizziness, it is advisable to seek medical attention promptly for proper evaluation and treatment.
What diagnostic tests are commonly used to identify whiplash-related headaches and associated symptoms that patients experience?
Medical professionals may use imaging tests such as X-rays, CT scans, or MRI scans to assess potential injuries to the neck and head that could be causing the whiplash-related headaches.
Are there non-pharmacological treatment options available to help patients experience managing whiplash headaches?
Yes, non-pharmacological treatments like physical therapy, chiropractic care, acupuncture, and relaxation techniques can be effective in managing whiplash-related headaches by addressing muscle tension and promoting healing.